You just increased your semaglutide dose from 0.5 mg to 1.0 mg. The next morning, waves of nausea hit before you finish breakfast. Yes, nausea is the most common side effect of semaglutide. It affects 44.2% of users at the 2.4 mg dose. The drug activates GLP-1 receptors in your brain's nausea center and slows gastric emptying by 30-40%. Both effects trigger nausea. The condition is dose-dependent and temporary: 80% of users report minimal or no nausea by 6-8 weeks at their final dose.
The STEP 1 trial reported nausea in 44.2% of semaglutide users versus 17.4% on placebo. Only 4.5% discontinued due to GI side effects (Wilding et al., NEJM 2021).
| Quick Reference | Details |
|---|---|
| Prevalence | 44.2% during titration, 10-15% at maintenance |
| Cause | GLP-1 receptor activation in area postrema + delayed gastric emptying |
| Onset | 24-72 hours after each dose increase |
| Worst transition | 0.5 mg to 1.0 mg |
| Resolution | 2-4 weeks at each stable dose |
| Key prevention | Follow the 4-week titration schedule strictly |
| Evidence level | Human clinical trials (STEP 1, STEP 2) |
For dosing protocols, see our semaglutide dosage chart. For safety information, see our peptide safety guide.
Get your custom peptide protocol:
- Tailored to your body and goals
- Precise dosing and cycle length
- Safe stacking combinations
- Backed by peer-reviewed studies
- Ready in under 2 minutes
What Causes Nausea on Semaglutide?
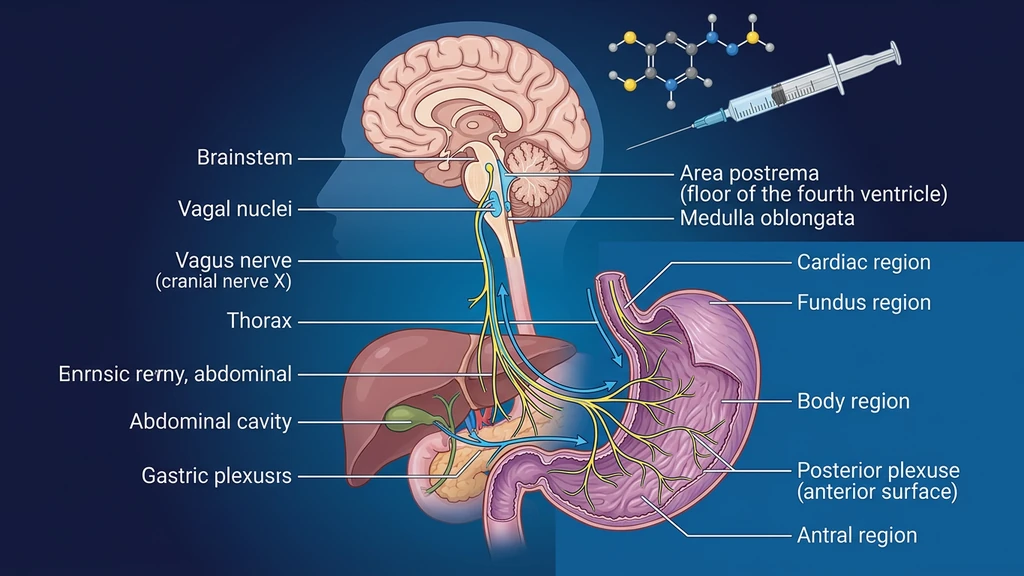
Think of your stomach like a washing machine. Semaglutide puts it on the slowest spin cycle. Food that normally clears in 2 hours now takes 3-4. The extra dwell time stretches the stomach wall, and your brain reads that stretch as a signal to stop eating. The same signal, pushed further, becomes nausea.
That is the peripheral mechanism: delayed gastric emptying. The central mechanism is more direct. Semaglutide activates GLP-1 receptors in the area postrema, a brain region that controls the vomiting reflex. It responds to the drug the way it responds to a toxin. Both pathways firing at once is why nausea dominates the early weeks.
A comprehensive review confirmed that GLP-1 agonists slow gastric emptying by 30-40% through vagal nerve pathways. This effect partially attenuates over 4-8 weeks, explaining why nausea improves at a stable dose (Nauck et al., 2021).
What Happens If You Skip Dose Levels
A user skipped the 0.5 mg dose and jumped from 0.25 mg straight to 1.0 mg. That is a 4x dose increase in one step instead of 2x. Nausea was so severe they vomited for 3 consecutive days and stopped the drug entirely. They never reached a therapeutic dose.
The standard titration exists for a reason: 0.25 mg for 4 weeks, then 0.5 mg for 4 weeks, then 1.0 mg. Each step roughly doubles the dose, giving the brain's GLP-1 receptors time to adapt. Skipping a level doubles the nausea severity. The STEP 2 trial in type 2 diabetes showed a lower nausea rate (33.6% vs 44.2%) partly because some investigators used slower titration (Davies et al., 2021).
A second scenario: a user ate a large steak dinner at a new dose level. With gastric emptying slowed by 35%, the meal sat in their stomach for over 5 hours. The gastric distension triggered severe nausea and vomiting. Switching to 4-5 small meals per day eliminated the episodes within 48 hours.
When Does Semaglutide Nausea Start and Stop?
Nausea follows a predictable pattern tied to dose changes.
Onset: 24-72 Hours After Each Dose Change
Nausea appears within 1-3 days of the first injection or each dose increase. The brain's GLP-1 receptors respond quickly. The 0.5 mg to 1.0 mg transition is typically the worst because it represents the largest proportional increase.
Peak: Days 2-5
Nausea is strongest in the first week at each new dose. Users describe it as constant low-grade queasiness, similar to mild motion sickness. It worsens after meals, especially large or fatty ones. By day 7, the intensity starts dropping.
Resolution: 2-4 Weeks at a Stable Dose
The brain adapts to sustained GLP-1 levels. After 4-6 weeks at the same dose, nausea drops substantially. For a detailed breakdown of resolution timelines across all side effects, see how long do semaglutide side effects last. At maintenance, only 10-15% report ongoing nausea compared to 40-45% during titration. About 80% of users have minimal symptoms by 6-8 weeks at their final dose.
When to Seek Medical Help
Vomiting more than 3 times per day, inability to keep fluids down for 24+ hours, nausea preventing eating for more than 2 days, or severe abdominal pain (possible pancreatitis). Persistent vomiting causes dehydration and electrolyte imbalances that require medical intervention.
How to Manage Nausea on Semaglutide
Five strategies reduce semaglutide nausea. The first one matters more than the other four combined.
Follow the Titration Schedule
Start at 0.25 mg. Increase every 4 weeks. Do not skip levels. If nausea is intolerable at a new dose, stay at the current level for an extra 4 weeks before trying again. There is no penalty for going slowly. The weight loss still happens at lower doses. Some users find that microdosing semaglutide at sub-standard doses reduces nausea while maintaining appetite suppression.
Eat Smaller, More Frequent Meals
Switch from 2-3 large meals to 4-5 smaller ones. With gastric emptying slowed by 30-40%, a full plate sits in your stomach far longer than usual. Smaller portions reduce distension and the nausea reflex. Stop eating before you feel full. Semaglutide amplifies fullness signals beyond what you expect.
Avoid Fatty and Fried Foods
Fat takes the longest to digest. During titration, favor lean proteins, complex carbs, and cooked vegetables. Greasy, fried, and rich foods are the most common nausea triggers. Many users find that a low-fat diet during the first month at each new dose eliminates most episodes.
Stay Upright After Eating
Do not lie down for 30 minutes after meals. Gravity helps food move from stomach to small intestine. Lying down traps food in a slow-emptying stomach and intensifies nausea. A gentle 10-minute walk after dinner helps by stimulating gastric motility.
Use Ginger or Anti-Nausea Medication
Ginger (250 mg capsules, 3-4 times daily, or fresh ginger tea) reduces nausea with clinical evidence. For severe cases, ondansetron (Zofran) 4-8 mg blocks serotonin receptors in the vomiting reflex. No drug interactions with semaglutide. Use short-term during dose escalation, not as a crutch to escalate faster.
What Does the Research Say?
STEP 1 Trial (Wilding et al., 2021) 1,961 participants. Nausea in 44.2% semaglutide versus 17.4% placebo. Most cases mild to moderate (grade 1-2). Only 4.5% discontinued due to GI effects. Nausea concentrated during titration, decreasing over time (PubMed).
STEP 2 Trial (Davies et al., 2021) Type 2 diabetes participants. Nausea in 33.6%, lower than STEP 1. Slower titration likely explains the difference. Confirmed area postrema GLP-1 receptors as the primary driver (PubMed).
Mechanistic Review (Nauck et al., 2021) GLP-1 agonists slow gastric emptying by 30-40% via vagal nerve pathways. Effect partially attenuates over 4-8 weeks. Attenuation is incomplete, which is why appetite suppression persists long-term even after nausea resolves (PubMed).
Important Warnings
Persistent vomiting (3+ episodes daily) can cause dehydration, electrolyte imbalances, and in rare cases acute kidney injury. If you cannot keep liquids down for 24 hours, contact your prescriber or seek urgent care.
Semaglutide is contraindicated with a history of pancreatitis. Severe abdominal pain radiating to the back alongside nausea may indicate pancreatitis (0.1-0.3% incidence). This requires immediate medical evaluation.
Do not fast thinking it will reduce nausea. A small, bland meal before or shortly after injection often helps. Complete fasting worsens nausea for many users. If nausea is contributing to a weight loss stall, see not losing weight on semaglutide for guidance.
Nausea that worsens after 6+ weeks at the same dose is atypical. Because semaglutide stays in your system for about five weeks, persistent nausea may reflect drug accumulation at steady state. This may indicate gastroparesis (severe delayed emptying) requiring dose reduction.
Related Side Effects
Does Semaglutide Cause Hair Loss? Severe nausea reduces food intake, deepening the caloric deficit that triggers telogen effluvium (hair shedding) in 3-5% of users. Controlling nausea helps maintain adequate nutrition.
Does Semaglutide Cause Fatigue? Nausea-driven reduced intake contributes to the fatigue that 11% of users experience. Both symptoms share a nutritional root cause.
Does Tirzepatide Cause Constipation? The same GLP-1 mechanism that causes nausea (slowed gut transit) drives constipation in both semaglutide and tirzepatide. Managing one often helps the other. If considering a switch, see semaglutide to tirzepatide conversion for dose equivalence.
Frequently Asked Questions
How long does semaglutide nausea last?
Nausea peaks within 2-5 days of each dose increase and improves within 2-4 weeks at a stable dose. By 6-8 weeks at your maintenance dose, roughly 80% of users report minimal or no nausea. The 4-week titration intervals exist to give your brain time to adapt at each level.
Does Ozempic cause more nausea than Wegovy?
Ozempic (max 2.0 mg) and Wegovy (2.4 mg) are the same molecule. Higher doses produce more nausea. Since Wegovy reaches 2.4 mg, users at maximum Wegovy dose experience slightly more nausea than maximum Ozempic users. At equivalent doses, nausea rates are identical.
Can I take Zofran with semaglutide?
Yes. Ondansetron (Zofran) 4-8 mg is commonly prescribed alongside semaglutide during titration. It blocks serotonin 5-HT3 receptors in the vomiting reflex. No known drug interactions with semaglutide. Your prescriber can provide a short-term supply for dose escalation periods.
Will eating before my semaglutide injection reduce nausea?
Many users find a small, bland meal 30-60 minutes before injection helps. Others do better injecting before bed so nausea occurs during sleep. Try one timing for 4 weeks, then switch if needed. The injection does not need to coincide with meals. Timing does not affect weight loss.
Is nausea a sign that semaglutide is working?
No. Nausea indicates your brain's area postrema is responding to GLP-1 activation, but weight loss does not correlate with nausea severity. Some users lose significant weight with minimal nausea. Others experience strong nausea with modest loss. Nausea is a side effect, not an efficacy marker.
The Bottom Line
Semaglutide nausea affects 4 in 10 users during titration but drops to 10-15% at maintenance. The two drivers: GLP-1 receptor activation in the brain's nausea center and 30-40% slower gastric emptying. Both partially attenuate as the body adapts.
Follow the titration schedule. Do not skip dose levels. Eat smaller meals, avoid fat during the first weeks at each new dose, and use ginger or ondansetron for acute episodes. Nausea persisting beyond 6 weeks at the same dose warrants medical evaluation.
Use our semaglutide dosage calculator to plan your titration. For dosing details, see our semaglutide dosage chart in mL. For a complete week-by-week timeline of what to expect during treatment, read how long does semaglutide take to work.
Related Articles: - Does Semaglutide Need to Be Refrigerated? — improper storage can worsen GI side effects - Does Semaglutide Expire? — degraded peptide may cause more nausea - How Much Bacteriostatic Water for Semaglutide? — correct mixing prevents concentration errors - Does Tirzepatide Cause Diarrhea? — related GI side effect across GLP-1 class - Best Peptides for Weight Loss — compare options if nausea is intolerable - How to Microdose Semaglutide — low-dose protocol to reduce GI side effects - Compound Semaglutide With B12 — compounded formulations with added B12
Related Articles
Does Semaglutide Cause Heartburn?
Semaglutide causes heartburn in 1.9-5% of users depending on dose. Learn the delayed gastric emptying mechanism, GERD vs heartburn differences, and 7 management strategies backed by clinical data.
Can Semaglutide Cause Diarrhea?
Diarrhea affects 8-30% of semaglutide users depending on dose. Learn the GLP-1 mechanism, STEP trial incidence data, timeline, and 6 management strategies.
Semaglutide Side Effects Duration
Most semaglutide side effects resolve within 2-4 weeks as your body adjusts. See clinical timelines for nausea, diarrhea, constipation, and fatigue.
Can Semaglutide Cause Depression?
Clinical trials show semaglutide does not increase depression risk. FDA cleared GLP-1 drugs of suicidality concerns in 2025. Evidence and mechanisms.