You have been injecting semaglutide for 8 weeks. The scale has not moved. Your coworker lost 12 pounds in the same timeframe on the same drug. You are wondering if you got a bad batch, if it does not work for you, or if something else is wrong. Most people who stall on semaglutide have a fixable problem, not a biological dead end. Clinical data from the STEP 1 trial shows 93.5% of participants lost at least 5% body weight at 68 weeks, but 6.5% did not reach even that threshold (Wilding et al., 2021). The real question is whether you are in that small non-responder group or whether something correctable is blocking your progress.
| Quick Reference | Details |
|---|---|
| Expected weight loss | 14.9% of body weight at 68 weeks (STEP 1) |
| Non-responder rate | 5-10% lose less than 5% body weight |
| Common plateau window | Weeks 8-12 |
| Most common fixable cause | Caloric intake still too high (metabolic adaptation) |
| BMR reduction with weight loss | 10-15% below predicted |
| Time to maximum effect | 16-20 weeks at maintenance dose (2.4 mg) |
| Alternative if non-responsive | Tirzepatide (22.5% weight loss in SURMOUNT-1) |
| When to reassess | After 16 weeks at maximum tolerated dose |
Use the semaglutide dosage calculator to verify your current dose is correct for your vial concentration. For a visual dosing reference, see the semaglutide dosage chart in mL.
Get your custom peptide protocol:
- Tailored to your body and goals
- Precise dosing and cycle length
- Safe stacking combinations
- Backed by peer-reviewed studies
- Ready in under 2 minutes
The Weight Loss Timeline Most People Get Wrong
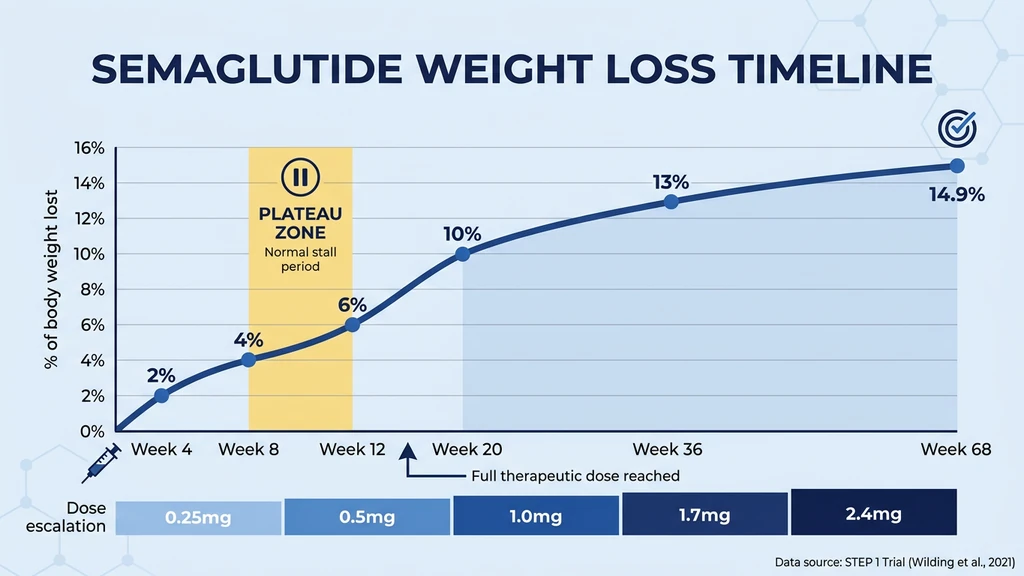
Semaglutide does not work like a light switch. It works like a thermostat slowly dialing down to a new set point. The titration schedule alone takes 16-20 weeks to reach the maximum dose of 2.4 mg. Judging the drug at week 4 on a 0.25 mg starting dose is like judging a marathon runner's pace during their warm-up lap.
For a visual comparison of real clinical outcomes month by month, see semaglutide before and after results. The STEP 1 trial mapped weight loss across 68 weeks. Here is what actually happened:
| Timepoint | Average Weight Loss | What Is Happening |
|---|---|---|
| Week 4 | 1.5-2% | Starting dose (0.25 mg); appetite may not change yet |
| Week 8 | 3-4% | Dose at 0.5 mg; appetite suppression begins |
| Week 12 | 5-7% | Dose at 1.0 mg; first plateau is common here |
| Week 20 | 9-11% | Reaching maintenance dose (2.4 mg) |
| Week 36 | 12-14% | Approaching maximum effect |
| Week 68 | 14.9% | Average end-of-trial result |
The plateau at weeks 8-12 catches nearly everyone off guard. Weight drops steadily for the first two months, then stops. Panic sets in. But this stall is a normal biological recalibration. Your body detects the energy deficit and temporarily adjusts metabolic rate, water retention, and hormonal output to resist further loss. The pause typically lasts 2-4 weeks before weight loss resumes at the next dose level.
A second common mistake is confusing weight loss rate with total weight loss. Semaglutide produces faster losses in the first 12 weeks and slower losses thereafter. Losing 2 pounds per week in month 1 and then 0.5 pounds per week in month 4 is the expected trajectory, not a sign of failure. The STEP 5 extension trial confirmed that weight loss continues gradually through week 104 in users who stay on the drug (Garvey et al., 2022).
If you are still in the titration phase (below 2.4 mg), you have not yet given the drug its full chance to work. Use the semaglutide dosage chart to confirm where you sit on the titration ladder. For a detailed breakdown of what to expect at each stage, see how long does semaglutide take to work.
8 Reasons Semaglutide Is Not Working for You
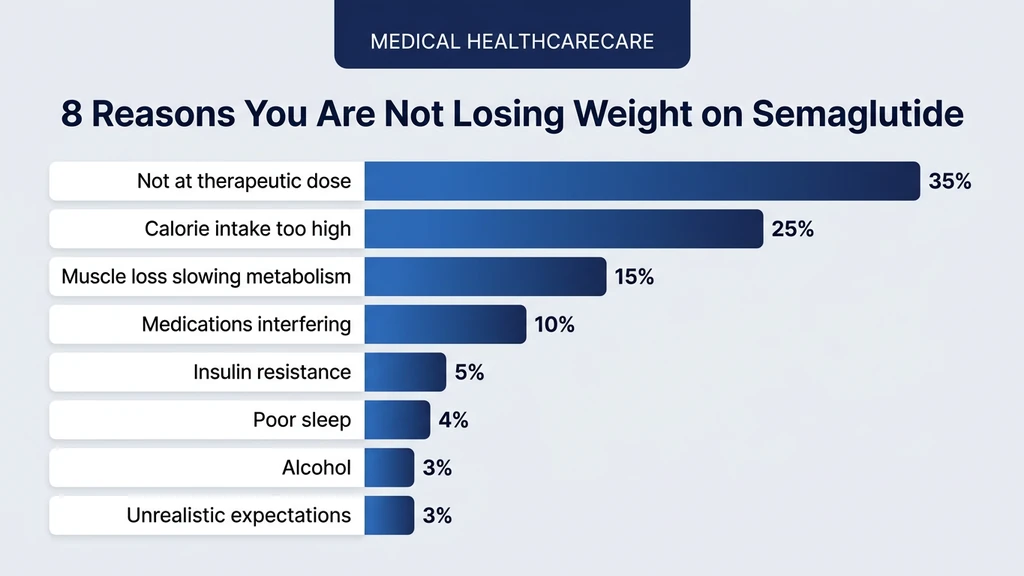
Each of these eight reasons has a specific mechanism and a specific fix. Most people who stall on semaglutide have at least two of these happening simultaneously. Read through all eight before deciding which apply to you.
1. Your Dose Is Too Low or You Are Titrating Too Slowly
The standard titration for Wegovy starts at 0.25 mg and increases every 4 weeks: 0.25, 0.5, 1.0, 1.7, then 2.4 mg. At the starting dose, the drug is not expected to produce significant weight loss. It exists to train your GI system to tolerate the medication.
Some providers extend each dose step to 6 or 8 weeks to minimize nausea. That is medically reasonable, but it means you may not reach the therapeutic dose for 5-6 months. During that stretch, weight loss will be slower than the clinical trial averages because those trials used the standard 4-week escalation.
The fix: Confirm with your provider that you are on the standard titration schedule. If GI side effects are minimal at your current dose, ask about moving to the next step on schedule rather than extending unnecessarily. The semaglutide dosage calculator converts your target milligram dose into syringe units for your specific vial concentration. If you are unsure how units translate to milligrams, our guide on how many mg is 40 units of semaglutide walks through the math.
The STEP 1 participants who lost the most weight were those who reached 2.4 mg by week 16 and stayed there. Delayed titration is not dangerous, but it does delay results.
2. You Have Not Given It Enough Time (The Week 8-12 Plateau)
A weight loss stall between weeks 8 and 12 is so predictable that researchers expect it. It occurs because your body's metabolic defense system activates in response to the caloric deficit.
Think of it like a thermostat. You set the temperature to 68 degrees. The system blasts cool air until it hits 68, then the compressor clicks off. Your body does the same. It detects a 500-calorie deficit, loses weight for 6-8 weeks, then adjusts metabolic output downward until the energy equation rebalances. This is not semaglutide failing. This is your metabolism doing what evolution designed it to do.
The fix: Do nothing. If you are still titrating up, the next dose increase will break through the plateau. If you are already at 2.4 mg, wait 4 more weeks. The STEP 1 data shows weight loss resumes in most participants after the initial plateau (Wilding et al., 2021). Changing your diet, exercise, or medication during a plateau introduces too many variables to identify what is actually working.
3. Your Caloric Intake Is Still Too High
Semaglutide reduces appetite. It does not eliminate it. If your meals shrink by 300 calories but you still consume 2,200 calories daily while your maintenance level is 2,000, you will not lose weight. The drug closed the gap but did not create a deficit.
This is the most common fixable reason for stalled weight loss on semaglutide. A study on GLP-1 agonist users found that self-reported caloric intake was 30-40% lower than actual measured intake (Lichtman et al., 1992). People underestimate what they eat. Liquid calories (juice, alcohol, coffee drinks), cooking oils, and snacking between meals are the usual culprits.
The fix: Track every calorie for 7 consecutive days using a food scale and a tracking app. Do not guess portions. Weigh them. If your daily average exceeds your maintenance calories minus 500, that is your answer. A 500-calorie daily deficit produces approximately 1 pound of fat loss per week. Anything smaller produces slower loss that may be masked by water fluctuations on the scale.
For reference, semaglutide reduced caloric intake by approximately 35% in the STEP 1 trial. If you are not experiencing meaningful appetite suppression, your dose may be too low or you may be eating around the appetite suppression (eating out of habit or boredom rather than hunger).
4. Muscle Loss Is Reducing Your Metabolic Rate
Here is a number that matters: for every pound of muscle you lose, your resting metabolic rate drops by approximately 6-7 calories per day (Wang et al., 2010). Lose 10 pounds of muscle, and your body burns 60-70 fewer calories daily at rest. Over a year, that deficit adds up to 7 pounds of potential fat loss that never happens.
Semaglutide causes weight loss that is approximately 60-65% fat and 35-40% lean mass in participants who do not exercise (Wilding et al., 2021). That lean mass loss includes muscle. A person who loses 30 pounds may have lost 10-12 pounds of muscle along with 18-20 pounds of fat. Their metabolic rate has dropped, their caloric deficit has shrunk, and weight loss stalls.
The fix: Resistance training 2-3 times per week and protein intake of 0.7-1.0 grams per pound of body weight. The combination preserves muscle during caloric restriction. A study on semaglutide plus exercise showed significantly better body composition outcomes than semaglutide alone (Lundgren et al., 2024). You do not need to become a powerlifter. Three sessions of basic compound movements (squats, deadlifts, presses, rows) for 30-40 minutes each is sufficient.
If you are experiencing unusual fatigue alongside your plateau, muscle loss may be contributing. See our article on semaglutide and fatigue for management strategies.
5. Medication Interactions Are Blunting the Effect
Several common medications reduce semaglutide's effectiveness or cause weight gain that offsets the weight loss.
Medications that may cause weight gain: - Insulin and sulfonylureas (diabetes medications that promote fat storage) - Beta-blockers (reduce metabolic rate by 5-10%) - SSRIs and SNRIs (weight gain in 25-30% of users after 6 months) - Corticosteroids (increase appetite and promote visceral fat deposition) - Antihistamines (central appetite stimulation)
Medications that may reduce semaglutide absorption: - Proton pump inhibitors (alter gastric pH, potentially affecting subcutaneous absorption kinetics) - Orlistat (fat malabsorption may alter GLP-1 signaling)
The fix: Review every medication you take with your prescriber. Do not stop any medication on your own. Ask specifically whether any of your current medications are associated with weight gain and whether alternatives exist. In the STEP 2 trial of semaglutide for type 2 diabetes, participants on insulin and sulfonylureas lost less weight (9.6% vs 14.9% in STEP 1) partly because those medications promote weight gain (Davies et al., 2021).
For a broader understanding of drug interactions, see our peptide safety guide.
6. Undiagnosed or Undertreated Thyroid Issues
Your thyroid controls metabolic rate. Hypothyroidism (underactive thyroid) reduces resting metabolic rate by 15-40%, depending on severity (Mullur et al., 2014). Subclinical hypothyroidism, where TSH is elevated but free T4 remains normal, affects 4-10% of adults and often goes undiagnosed. It creates enough metabolic drag to stall weight loss on semaglutide.
A person with a TSH of 6.0 (normal range: 0.4-4.0) may have a resting metabolic rate 100-200 calories below what it should be. Over 16 weeks, that deficit gap translates to 3-5 fewer pounds lost. Enough to make the difference between feeling like semaglutide is working and feeling like it is not.
The fix: Get a thyroid panel (TSH, free T4, free T3) if you have not had one in the past year. Symptoms that overlap with semaglutide side effects include fatigue, cold intolerance, constipation, and dry skin. If your TSH is above 4.0, discuss treatment with your provider. Optimizing thyroid function may restore the weight loss that semaglutide is supposed to produce. For more on semaglutide and fatigue overlap, read does semaglutide cause fatigue.
7. Sleep Deprivation and Cortisol Are Working Against You
Sleeping less than 6 hours per night increases ghrelin (the hunger hormone) by 14.9% and decreases leptin (the satiety hormone) by 15.5% (Spiegel et al., 2004). Those hormonal shifts directly counteract semaglutide's appetite suppression mechanism. You are fighting the drug with your schedule.
Chronic sleep deprivation also elevates cortisol. Elevated cortisol promotes visceral fat storage, increases insulin resistance, and triggers cravings for high-calorie foods. A study found that sleep-restricted adults consumed an additional 385 calories per day compared to well-rested controls (Al Khatib et al., 2017). Those 385 calories can wipe out the entire deficit semaglutide creates.
The fix: Aim for 7-9 hours of sleep per night. If semaglutide is causing nausea that disrupts sleep, switch your injection day to the morning so that peak nausea (24-48 hours post-injection) falls during waking hours rather than at bedtime. See our article on semaglutide and nausea for additional management strategies.
Track your sleep for two weeks alongside your weight. If you consistently sleep under 6 hours and the scale is not moving, fixing sleep may matter more than adjusting the drug.
8. Severe Insulin Resistance Is Slowing Your Response
Insulin resistance creates a metabolic headwind that semaglutide must overcome before weight loss begins. In the STEP 2 trial (participants with type 2 diabetes and higher average insulin resistance), mean weight loss was 9.6% at 68 weeks, compared to 14.9% in the non-diabetic STEP 1 population (Davies et al., 2021). That 5.3 percentage point gap is almost entirely attributable to baseline insulin resistance.
Think of insulin resistance like driving with the parking brake engaged. The engine (semaglutide) is running. The car moves. But it moves slower than it should because there is friction that the engine was not designed to overcome on its own.
Markers of insulin resistance include fasting insulin above 15 mIU/L, HOMA-IR above 2.5, HbA1c above 5.7%, and waist circumference above 40 inches (men) or 35 inches (women). The more elevated these markers, the slower initial weight loss will be.
The fix: Insulin resistance responds to exercise (especially resistance training and high-intensity intervals), reduced refined carbohydrate intake, and time. Semaglutide itself improves insulin sensitivity over weeks to months, which means the drug's effectiveness may increase the longer you take it. Participants in STEP 2 who stayed on semaglutide for 68 weeks continued to improve glycemic markers throughout, suggesting the metabolic headwind weakens over time. If insulin resistance is severe, your provider may consider tirzepatide, which targets both GLP-1 and GIP receptors and shows stronger effects on insulin sensitivity (Frias et al., 2021).
The Metabolic Adaptation Problem
Your body fights weight loss. This is not a theory. It is a measured, quantified biological response that researchers call metabolic adaptation or adaptive thermogenesis.
When you lose weight, your resting metabolic rate drops more than the weight loss alone would predict. A 200-pound person with a BMR of 1,800 calories loses 30 pounds. You would expect their BMR to drop to approximately 1,620 (proportional to the weight loss). Instead, it may drop to 1,530 or lower. That extra 90-calorie drop is metabolic adaptation, and it is the reason weight loss slows and eventually stops if the caloric deficit is not adjusted (Rosenbaum et al., 2010).
The magnitude is significant: 10-15% below the predicted BMR based on new body weight. The Biggest Loser study documented metabolic rates 500+ calories below predicted levels 6 years after weight loss in contestants who lost extreme amounts rapidly (Fothergill et al., 2016). While semaglutide users lose weight more gradually, the same mechanism applies at a smaller scale.
How metabolic adaptation stalls semaglutide weight loss:
| Factor | Before Semaglutide | After 20 lbs Lost | Net Effect |
|---|---|---|---|
| BMR | 1,800 cal/day | 1,550 cal/day (-250 actual vs -180 predicted) | 70 fewer calories burned than expected |
| NEAT (fidgeting, walking) | 400 cal/day | 300 cal/day | 100 fewer calories burned |
| TEF (thermic effect of food) | 200 cal/day | 160 cal/day | 40 fewer calories burned |
| Exercise calories | 300 cal/day | 250 cal/day (same exercise feels harder) | 50 fewer calories burned |
| Total daily expenditure | 2,700 cal/day | 2,260 cal/day | 440 fewer calories burned |
That 440-calorie reduction means the deficit that was producing 1 pound per week of fat loss is now producing 0.1 pounds per week. The scale appears frozen. You feel like semaglutide stopped working. In reality, your body adjusted its energy output to match the reduced input.
The countermeasures are straightforward but require effort. Resistance training maintains or builds muscle, keeping BMR higher. Increasing daily movement (walking 8,000-10,000 steps) preserves NEAT. Eating adequate protein (0.7-1.0g per pound of body weight) maintains the thermic effect of food. These interventions do not eliminate metabolic adaptation, but they reduce its magnitude from 15% to 5-8%, which is enough to keep weight loss moving.
For a comprehensive overview of weight loss peptides and how different compounds approach the metabolic adaptation problem, see our weight loss guide.
What the Clinical Trials Actually Show
The marketing around semaglutide emphasizes the average results. But averages hide enormous variation. Here is what the full data set reveals across four major trials.
STEP 1 (Non-Diabetic Obesity) 1,961 participants. 2.4 mg semaglutide weekly for 68 weeks. Average weight loss: 14.9% of body weight (vs 2.4% placebo). But 6.5% of semaglutide participants lost less than 5% of body weight, the threshold below which most guidelines consider treatment unsuccessful. The top 25% of responders lost more than 20%. The bottom 25% lost less than 10% (Wilding et al., 2021).
STEP 2 (Type 2 Diabetes) 1,210 participants. Same drug, same dose. Average weight loss: 9.6%. The 5.3 percentage point gap versus STEP 1 is driven by insulin resistance, concurrent diabetes medications that promote weight gain, and higher baseline metabolic dysfunction. Approximately 12% of participants lost less than 5% (Davies et al., 2021).
STEP 3 (Intensive Behavioral Therapy + Semaglutide) 611 participants receiving semaglutide plus intensive behavioral therapy (meal replacements, exercise coaching, counseling). Average weight loss: 16.0%. The 1.1 percentage point improvement over STEP 1 shows that behavioral intervention adds modest benefit on top of the drug alone. But the non-responder rate dropped to approximately 4%, suggesting that coaching helped people avoid the fixable mistakes outlined above (Wadden et al., 2021).
STEP 4 (Withdrawal Study) 902 participants who had already lost weight on semaglutide for 20 weeks were randomized to continue or switch to placebo. Those who continued lost an additional 7.9%. Those who switched to placebo regained 6.9%. This trial proved that semaglutide's weight loss effect is ongoing: the drug must be continued for weight maintenance (Rubino et al., 2021).
What the non-responder data means for you:
If you have been on semaglutide 2.4 mg for at least 16 weeks, you have had adequate time and dose exposure to evaluate the drug. Less than 5% body weight loss at that point puts you in the non-responder category. But verify the 8 reasons above first. True biological non-response (where the drug genuinely does not activate your GLP-1 receptors adequately) is rare. Most non-response is actually under-dosing, insufficient time, or a correctable behavioral or medical factor.
For a full comparison of GLP-1 and multi-agonist peptides, see our articles on retatrutide and the retatrutide vs tirzepatide comparison.
When to Consider Switching to Tirzepatide
Tirzepatide targets two receptors (GLP-1 and GIP) instead of one. The additional GIP agonism provides enhanced insulin sensitization, greater appetite suppression, and improved fat oxidation that semaglutide's single-receptor mechanism cannot match.
The numbers tell the story clearly:
| Metric | Semaglutide 2.4 mg (STEP 1) | Tirzepatide 15 mg (SURMOUNT-1) |
|---|---|---|
| Mean weight loss | 14.9% | 22.5% |
| Participants losing >20% | ~25% | ~57% |
| Participants losing <5% | ~6.5% | ~3% |
| Trial duration | 68 weeks | 72 weeks |
| Mechanism | GLP-1 only | GLP-1 + GIP dual agonist |
The SURMOUNT-1 trial enrolled 2,539 non-diabetic adults with obesity. At the highest dose (15 mg), 57% of participants lost more than 20% of body weight. The non-responder rate (less than 5% loss) was approximately 3%, roughly half the rate seen with semaglutide.
When switching makes sense: - You have been on semaglutide 2.4 mg for 16+ weeks with less than 5% weight loss - You have addressed all fixable factors (calories, exercise, sleep, thyroid, medications) - Your provider agrees that a medication change is appropriate
When switching does not make sense: - You are still titrating semaglutide (have not reached 2.4 mg) - You have been at maintenance dose for less than 12 weeks - You have not tracked calories or addressed lifestyle factors - Your weight loss has stalled but you have lost more than 10% total (this is metabolic adaptation, not non-response)
The switching protocol involves stopping semaglutide, waiting one week for clearance (since semaglutide stays in your system for about five weeks, overlap is minimal at the one-week mark), and starting tirzepatide at the equivalent dose. For the complete dose conversion table and step-by-step instructions, see our semaglutide to tirzepatide switching guide. Use the tirzepatide dosage calculator to convert your new dose into syringe units. If you have already switched and want to know what timeline to expect, read why am I not losing weight on tirzepatide for the tirzepatide-specific troubleshooting protocol.
A third option exists for true non-responders to both semaglutide and tirzepatide. Retatrutide, a triple agonist (GLP-1 + GIP + glucagon receptor), produced 24.2% weight loss at 48 weeks in Phase 2 trials (Jastreboff et al., 2023). It is still in clinical trials and not yet FDA-approved, but it represents the next step for patients who do not respond to dual agonism. Learn more in our retatrutide vs tirzepatide comparison.
For cost comparisons between these medications, the peptide cost calculator estimates monthly expenses based on your dose and source.
A 4-Week Troubleshooting Protocol
If your weight has stalled on semaglutide, follow this protocol for 4 weeks before concluding the drug is not working. Each week targets a specific variable. By isolating one change at a time, you can identify exactly what is blocking your progress.
Week 1: Audit Your Calories and Protein
Buy a food scale. Download a tracking app. Log every single thing you eat and drink for 7 days. No estimating. No rounding. No skipping the handful of almonds or the splash of cream in your coffee.
Target numbers: - Daily calories: maintenance calories minus 500 (use an online TDEE calculator for your current weight) - Daily protein: 0.7-1.0 grams per pound of current body weight - Daily water: half your body weight in ounces (minimum 64 oz)
At the end of week 1, calculate your daily average. If your actual intake is higher than your target, you have found the problem. Adjust portions and move to week 2. If intake is already at or below target, the issue is elsewhere.
This single step resolves the stall for more than half of semaglutide users who report the drug is not working. The appetite suppression may be functioning perfectly while portion sizes remain unchanged out of habit.
Week 2: Add Resistance Training
Start a basic resistance training program. Three sessions, 30-40 minutes each. Focus on compound movements that work multiple muscle groups simultaneously.
Sample schedule: - Monday: Squats, bench press, bent-over rows (3 sets of 8-12 reps each) - Wednesday: Deadlifts, overhead press, lat pulldowns (3 sets of 8-12 reps each) - Friday: Lunges, dumbbell press, cable rows (3 sets of 8-12 reps each)
If you have never lifted weights, start with body weight or light dumbbells. The goal is not to build significant muscle in one week. The goal is to signal your body that muscle is needed, preventing further lean mass loss from the caloric deficit.
Resistance training also improves insulin sensitivity acutely. Each session opens glucose channels in muscle cells that remain active for 24-48 hours, reducing the metabolic headwind from insulin resistance. This effect is separate from and additive to semaglutide's own insulin-sensitizing action.
Week 3: Optimize Sleep and Stress
Track your sleep with a wearable or a simple bedtime/wake-time log. Calculate your average hours per night.
Action items: - If sleeping less than 7 hours: set a fixed bedtime that allows 7.5-8 hours in bed - If injection-related nausea disrupts sleep: move your injection to the morning - If stress is chronic: add 10-15 minutes of walking after dinner (reduces cortisol measurably within 1 week) - Remove screens from the bedroom 30 minutes before sleep - Keep the room at 65-68 degrees Fahrenheit
At the end of week 3, compare your average sleep duration to the previous two weeks. If sleep improved and weight started moving, you have identified the bottleneck. If sleep was already adequate, proceed to week 4.
For managing nausea that may be disrupting your routine, see our semaglutide nausea guide.
Week 4: Medical Review
Request the following blood tests from your provider:
Essential panel: - TSH and free T4 (thyroid function) - Fasting insulin and fasting glucose (calculate HOMA-IR) - HbA1c (3-month blood sugar average) - Complete metabolic panel (liver, kidney function) - Iron, ferritin, B12, vitamin D
Review with your provider: - Current medication list for weight-gain-promoting drugs - Whether your semaglutide dose can be increased (if below 2.4 mg) - Whether switching to tirzepatide is appropriate - Whether compound semaglutide with B12 might address micronutrient gaps - Whether compounding pharmacy semaglutide requires verification of potency
If all blood work is normal, you are eating at a 500-calorie deficit, exercising 3 times per week, sleeping 7+ hours, and have been at 2.4 mg for 16+ weeks with less than 5% weight loss, you may be a true pharmacological non-responder. This affects 5-10% of users. The next step is a medication change, not a behavior change. For a data-driven comparison of older appetite suppressants versus GLP-1 drugs, see our phentermine vs GLP-1 guide.
For proper handling and reconstitution of your medication, see our guide on how much bacteriostatic water for semaglutide. For general peptide dosage references, check our comprehensive chart.
Hair Loss, Fatigue, and Other Side Effects That Signal a Problem
Side effects are not just nuisances. They are diagnostic clues. Certain side effects that appear alongside a weight loss stall point to specific underlying causes.
Fatigue + weight stall: Likely caloric intake too low (below 1,000/day) or thyroid dysfunction. The body conserves energy by reducing metabolic rate and subjective energy. This is a protective mechanism, not a drug failure. Read more in does semaglutide cause fatigue.
Hair loss + weight stall: Telogen effluvium from rapid initial weight loss followed by a plateau. The hair loss reflects where your body was 2-3 months ago (the rapid loss phase), not your current state. It typically resolves on its own within 6-9 months. Ensure protein intake is above 0.7g per pound of body weight. See does semaglutide cause hair loss.
Persistent nausea + weight stall: If nausea is so severe that you cannot eat adequately, the resulting caloric deficit may be too extreme. Paradoxically, eating too little can stall weight loss through metabolic adaptation. Learn management strategies in does semaglutide cause nausea.
No appetite suppression at all: This is the strongest signal that the drug is not reaching therapeutic levels. Possible causes include degraded medication (improper storage), incorrect injection technique (injecting into muscle rather than subcutaneous fat), or genuine biological non-response. Verify your reconstitution with the bacteriostatic water mixing guide and review proper storage in our peptide safety guide.
None of these side effects require stopping semaglutide. Most semaglutide side effects resolve within predictable timelines, and each has a targeted solution that addresses the root cause without abandoning the medication.
Frequently Asked Questions
How long does semaglutide take to start working for weight loss?
Most users notice appetite suppression within 1-2 weeks, but meaningful weight loss (5%+ of body weight) typically takes 12-16 weeks. The full titration to 2.4 mg takes 16-20 weeks. The STEP 1 trial showed average weight loss of 5-7% at week 12 and 14.9% at week 68. Judge results at the maintenance dose, not during titration.
What percentage of people do not lose weight on semaglutide?
Approximately 6.5% of participants in the STEP 1 trial lost less than 5% of body weight at 68 weeks. True biological non-response, where the drug has no effect despite correct dosing and adherence, affects an estimated 5-10% of users. Most people who report failure have a correctable issue like insufficient dose, too much caloric intake, or medication interactions.
Can I lose weight on semaglutide without exercise?
Yes, but less effectively. STEP 1 participants lost 14.9% of body weight without a mandated exercise program. STEP 3 added behavioral therapy including exercise coaching and achieved 16.0%. Exercise preserves muscle mass, prevents BMR decline, and improves insulin sensitivity. Without it, approximately 35-40% of weight lost is lean mass rather than fat.
Why did I stop losing weight on Ozempic after 3 months?
A plateau at 8-12 weeks is biologically normal. Your body reduces metabolic rate, increases water retention, and adjusts hormonal output to resist further weight loss. If you are still titrating, the next dose increase will likely break through. If you are at maintenance dose, wait 4 more weeks. Persistent stalls beyond 16 weeks at max dose warrant medical evaluation.
Is tirzepatide better than semaglutide for weight loss?
Clinical trial data suggests yes. SURMOUNT-1 showed 22.5% weight loss with tirzepatide 15 mg versus 14.9% with semaglutide 2.4 mg in STEP 1. Tirzepatide's dual GLP-1/GIP mechanism provides additional appetite suppression and insulin sensitization. However, individual response varies. Some patients respond well to semaglutide and poorly to tirzepatide.
Does semaglutide work if you have insulin resistance?
Yes, but more slowly. STEP 2 participants with type 2 diabetes (higher insulin resistance) lost 9.6% versus 14.9% in the non-diabetic STEP 1 group. Semaglutide itself improves insulin sensitivity over time, meaning results may accelerate as metabolic function improves. Adding resistance training and reducing refined carbohydrates can accelerate this process.
How do I know if my semaglutide is working?
Three signals confirm semaglutide is active: reduced appetite within 1-2 weeks, feeling full faster during meals, and decreased food-related thoughts. Weight loss may lag behind appetite changes by 2-4 weeks. If you experience zero appetite suppression after 4 weeks at 0.5 mg or higher, verify medication potency, injection technique, and storage conditions.
Should I eat less than 1,200 calories on semaglutide?
No. Eating below 1,200 calories daily accelerates muscle loss, triggers severe metabolic adaptation, increases fatigue, and raises the risk of gallstones. A 500-750 calorie deficit below your maintenance level is the target. If semaglutide suppresses appetite so much that you cannot eat 1,200 calories, discuss a dose reduction with your provider.
The Bottom Line
Semaglutide works for the overwhelming majority of people who take it at the right dose for enough time. The STEP trial program proved that. But "works" does not mean identical results for everyone, and the path from injection to scale movement passes through calories, muscle mass, sleep, thyroid function, insulin resistance, and medication interactions.
Start with the 4-week troubleshooting protocol. Track your calories honestly for one week. Add resistance training. Fix your sleep. Get blood work. In that order. Most stalls resolve at step one or two without changing the medication at all.
If you have completed that protocol and remain below 5% weight loss after 16 weeks at 2.4 mg, a switch to tirzepatide is the evidence-based next step. Use the semaglutide to tirzepatide switching guide and the tirzepatide dosage calculator to plan the transition with your provider.
Calculate your current dose with the semaglutide dosage calculator. Compare costs with the peptide cost calculator.
Related articles: - Why Am I Not Losing Weight on Tirzepatide? — the parallel troubleshooting guide for tirzepatide users - How Long Does Semaglutide Take to Work? — week-by-week timeline with STEP trial data - Does Tirzepatide Burn Fat? — how the dual agonist drives fat loss vs lean mass loss - How Does Retatrutide Work? — the triple agonist delivering 28.7% weight loss in trials - Can You Drink Alcohol on Tirzepatide? — alcohol reduces fat oxidation by 73% and stalls GLP-1 weight loss - How to Reconstitute Tirzepatide — preparation guide for research peptide users - Semaglutide Before and After — month-by-month clinical results and visual timeline - How to Microdose Semaglutide — low-dose protocol for users sensitive to side effects
Explore all peptide profiles and research tools at PeptidesExplorer.com.
Related Articles
Not Losing Weight on Tirzepatide?
Not losing weight on tirzepatide? About 3% of users are non-responders. Learn 8 fixable reasons, SURMOUNT trial data, and a 4-week troubleshooting protocol.
Can You Drink on Semaglutide? Risks
Can you drink on semaglutide? No ban, but risks include hypoglycemia, prolonged intoxication, 73% fat-burn suppression, and worse GI side effects.
How to Get Semaglutide: Prescription, Cost, Access
Get semaglutide via prescription, telehealth, or pharmacy. BMI eligibility, insurance, brand vs. compounded costs, and access guide for 2026.
How Much Is Semaglutide? 2026 Cost Breakdown
Semaglutide costs $149-$1,349/month depending on formulation. Compare Wegovy, Ozempic, compounded, and oral prices with savings strategies.